Toothache can be of different types: some can be tolerated, and some reaches the level of extreme and measures should be taken immediately.
Any injury to the gums or teeth can be extremely painful. At other times, you might have dental pain and not know why. For instance, unexpected severe pain might be brought on by pieces of food that can be found in contact with a decayed area of the tooth. Food, heat or cold may create pressure near the nerve and cause pain. The nerve inside the tooth likewise might be exposed if you lose a filling or crown.
Extreme Tooth Pain: Causes
Pain that gets worse over time can also be triggered by food that’s stuck in between your tooth and gum. If you don’t brush and floss well, the bits of food stay. Bacteria multiply in this area, and an infection of the tooth and gum might develop. This kind of infection is called an abscess. It can be at the root end of the tooth (in bone) or in the gums. An abscess can be a severe illness if it is not treated.
Pro Tip: This Portable Water Flosser is up to 50% more effective than traditional floss and can save you hundreds on professional dental cleanings. Its 300ml tank and cordless design make it perfect for maintaining healthy gums. Check the current deal on Amazon.
Pain when you bite or chew can be a sign of an abscess, specifically if you likewise notice a bad odor or a bad taste in your mouth.
The majority of patients comprehend that conclusive care needs to be provided by a dental expert or oral surgeon, but either an absence of financial resources, failure to contact their dental professional, serious pain, or acute trauma leads patients to EDs first. While treating oral emergencies in the ED can be hard, challenging, and frustrating, it likewise can be profoundly satisfying when the emergency doctor has a basic understanding of oral anatomy and understands the simple strategies needed to eliminate pain and maintain teeth. Numerous emergency physicians are called upon to deal with oral issues, and it is essential to have a diagnostic and treatment plan to facilitate patient care.
Extreme Tooth Pain: Treatment
First, call your dentist and make an appointment.
Even when dental problems cause a lot of pain, the problems, and the treatments, often are fairly simple if you look for help immediately.
Dental Care: This Rotating Electric Toothbrush removes up to 400% more plaque than a manual brush. With a built-in pressure sensor and 8 replacement heads included (a 2-year supply), it’s a cost-effective way to maintain a professional clean at home. Available on Amazon.
The first thing your dental practitioner will do is take an X-ray. If you have a cavity, your dental practitioner will remove the decayed part of the tooth and place a filling. Once the inner part of the tooth is protected, the pain will normally vanish right away.
If your problem is associated with pieces of food stuck under your gums, your dental expert will get rid of the pieces. If you have an infection, you might be provided a prescription for antibiotics and pain medicine. Take your antibiotics precisely as directed, even if you begin to feel far better after just a day or more.
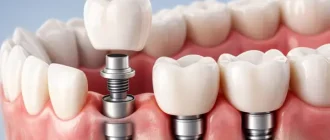
An abscess in the tooth will require root canal treatment. An abscess in the gum may need to be drained pipes. If the tooth is very damaged, it might have to be gotten rid of.
Short, sharp, shooting pain
This type of pain can be generalised or restricted to one area of the mouth. The pain may be due to fluid movement through open tubules in the dentine or there might be some initial inflammatory changes in the oral pulp. It can be brought on by caries, dentine exposure on root surface areas, divided cusp, lost or fractured remediation or a fractured tooth.
Patients complain typically of a sharp pain associated with hot, cold or sweet stimuli. The pain is just present when a stimulus is applied. When it comes to a cracked cusp, rough bread or tough food may produce a sharp pain, that might be spasmodic, on biting or chewing.
With gingival recession, recent scaling, or tooth wear due to a high acid diet or gastric reflux, there might be generalised dentine level of sensitivity. Nevertheless, with caries, fractured fillings and broken cusps, the pain tends to be localised to the affected tooth.
Intermittent sharp, shooting pains are likewise symptomatic of trigeminal neuralgia, so care should be taken not to mistakenly label toothache as neuralgia.
What to do
For root sensitivity making use of a desensitising toothpaste and a decrease in acid in the diet will help solve the symptoms. Making use of a fluoride mouth-rinse might also help. In the case of caries, a lost filling or fractured tooth, coverage of the exposed dentine with a temporary remediation will typically eliminate the symptoms.
Read also about how to relieve nerve pain in tooth.
Dull, throbbing, persistent pain
This type of pain might have a number of causes. These include tooth issues, food impaction, pericoronitis, acute necrotising ulcerative gingivitis, temporomandibular condition, or even maxillary sinusitus.
Painful tooth problems
The most common dental cause of dull, throbbing consistent pain is caries. Oftentimes this is recurrent and associated with an existing restoration. Where the pulp is impacted irreversibly, necrosis might follow with possible advancement of a periapical infection. A fractured cusp involving the pulp, or a large deep remediation may likewise be associated with this type of pain. Impacted teeth might hurt to percussion in the later stages of periapical inflammation.
There is substantial variation in the pain reported by patients, however it frequently starts as a sharp stabbing pain that becomes gradually dull and throbbing. In the beginning the pain might be triggered by a stimulus, but it then becomes spontaneous and stays for a considerable time after removal of the stimulus. The pain might radiate and be described other areas of the mouth. This type of pain tends to cause the patient to have problem sleeping and may be exacerbated by resting. Heat may make the pain even worse whereas cold may minimize it. The pain might be intermittent with no routine pattern and might have happened over months or years. If there is periapical infection present, patients might no longer complain of pain in response to a thermal stimulus, but rather of sensitivity on biting.
What to do
Treatment of affected teeth will involve either root canal therapy or tooth removal. In some patients, periapical inflammation can lead to a cellulitis of the face characterised by a rapid spread of bacteria and their breakdown items into the surrounding tissues triggering substantial oedema and pain. If systemic signs of infection exist, for example, fever and malaise, as well as swelling and potentially trismus (limitation of mouth opening), this is a surgical emergency situation. Antibiotic treatment alone is not suitable or suggested.
Should antibiotics be prescribed?
While antibiotics are suitable in the management of specific oral infections, they are not shown if the pain arises from inflammatory (non-infective) or neuropathic mechanisms. The degree of pain is not a reputable indication of acute infection.
There is proof that Australian dentists and medical professionals are using antibiotics empirically for dental pain, rather than making cautious diagnoses of the causes of the pain.1 Most oral emergency situation scenarios include patients with acute inflammation of the dental pulp or the periapical tissues. Prescribing antibiotics for these conditions will not get rid of the cause of the issue nor destroy the bacteria within the tooth.
Antibiotics must be restricted to patients with despair, fever, lymph node participation, a suppressed or compromised body immune system, cellulitis or a spreading infection, or a rapid onset of extreme infection.
If pus is present, it needs to be drained pipes, the cause eliminated, and host defences augmented with antibiotics. The microbial spectrum is primarily gram positive including anaerobes. Proper antibiotics would include a penicillin or a ‘first generation’ cephalosporin, combined with metronidazole in more severe cases.
Paracetamol or a non-steroidal anti-inflammatory drug is the suggested analgesic in the initial treatment of dental pain.
Food impaction and pericoronitis
Soft tissue problems that may trigger dull, throbbing, consistent pain consist of local inflammation (acute gingivitis connected with food impaction) or pericoronitis.
Chronic periodontitis with progressive bone loss, rarely triggers pain and patients might be unaware of the disorder until tooth mobility appears. There is quite often bleeding from the gums and sometimes an unpleasant taste. This is generally a generalised condition, however, deep stealing with extreme bone loss can occur around isolated teeth. Food impaction in these areas can trigger localised gingival pain. Poor contact in between nearby teeth and the existence of an occluding cusp forcing food into this space can likewise trigger a build-up of food debris and lead to gingival inflammation.
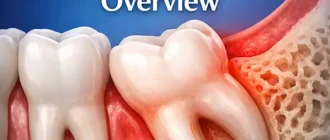
Acute pericoronitis involves bacterial infection around an unerupted or partly emerged tooth and usually affects the lower third molar (wisdom tooth). The condition is typically aggravated by the upper molar effecting on the swollen flap of soft tissue covering the unerupted tooth. There may be trismus.
What to do
Food particles should be gotten rid of and drainage established, if pus exists. Watering with chlorhexidine and rinsing the mouth with hot salty water is suggested. Early referral to a dentist is indicated. Cellulitis can establish, requiring immediate referral to a surgeon.
Acute necrotizing ulcerative gingivitis
Acute necrotising ulcerative gingivitis is a quickly progressive infection of the gingival tissues that triggers ulcer of the interdental gingival papillae. It can cause comprehensive destruction. Normally young to middle-aged people with minimized resistance to infection are impacted. Males are most likely to be affected than women, with stress, smoking cigarettes and poor oral hygiene being inclining aspects. Halitosis, spontaneous gingival bleeding, and a’ punched-out ‘look of the interdental papillae are very important signs.
The patients on a regular basis complain of severe gingival inflammation with pain on consuming and tooth brushing. The pain is dull, ingrained and continuous. The gums can bleed spontaneously and there is also an unpleasant taste in the mouth.
What to do
As there is an acute infection with generally anaerobic bacteria, treatment follows surgical principles and consists of shallow debridement, usage of chlorhexidine mouthwashes and a course of metronidazole pills. Treating the contributing aspects must prevent a recurrence.
Dry socket
A dull throbbing pain develops two to 4 days after a mandibular tooth extraction. It rarely happens in the maxilla. Smoking cigarettes is a major predisposing aspect as it decreases the blood supply. The tissue around the socket is very tender and white lethal bone is exposed in the socket. Halitosis is very common.
What to do
The area must be irrigated completely with warm saline service. If loose bone exists, local anaesthesia may be essential to allow thorough cleansing of the socket. Patients must be shown how to irrigate the area and told to do this regularly. Analgesics are shown, but pain may persist for several days. Although viewpoint is divided regarding whether or not dry socket is an infective condition, we do not advise making use of antibiotics in its management.
Temporomandibular disorders
Temporomandibular disorders might lead to pain that is confused with toothache. Patients usually experience unilateral vague pain occurring in the joint area and in the surrounding muscles of mastication. If the client bruxes (clenches or grinds) at night, then pain in the temporal area on waking is common. Patients who clench during the day might discover they get symptoms at the end of the day. The symptoms are frequently cyclical, solving then repeating once again. On questioning, patients will often be able to expose stressful occurrences that may have activated this procedure. Palpation of the muscles of mastication will elicit inflammation, typically unilaterally. There may also be inflammation around the temporomandibular joints, constraint in mouth opening and obvious wear of the teeth. This wear might add to dentine level of sensitivity, as the enamel is deteriorated by the tooth grinding. Wear elements will be seen on repairs along with natural teeth. On a regular basis, neck and shoulder muscles are tender to palpation. There may be joint pain with clicking and grating.
What to do
Reassurance about the self-limiting nature of the issue and its reversibility might be all that is needed. Anti-inflammatory drugs and muscle relaxants can likewise help. Building and construction of a night-guard and muscle exercises might be indicated consequently. These exercises may consist of gentle passive stretching, or resistance and clenching exercises.
Sinusitis
This is caused by infection of the maxillary sinus, usually following an upper respiratory tract infection. Nevertheless, there can be a history of recent tooth extraction leading to an oro-antral fistula. Patients typically complain of unilateral dull pain in all posterior upper teeth. All these teeth may hurt to percussion, but they will respond to a pulp sensitivity test. There are usually no other dental signs.
The pain tends to be increased on resting or flexing over. There is often a sensation of’ fullness’ on the affected side. The pain is usually unilateral, dull, throbbing and continuous. Frequently the patient feels unhealthy generally and feverish.
What to do
Pain stemming from the sinus develops generally from pressure. Decongestants can assist sinus drain. Antibiotics probably have only a bit part in moderate cases. Recommendation to an otorhinolaryngologist for endoscopic sinus surgery may be shown in chronic cases.
Home Remedies for Extreme Tooth Pain
Your head pounds, your gums throb, and your mouth aches and tender. You’ve got a toothache. See your dental professional ASAP. In the meantime, utilize these home remedies to get short-term relief.
Saltwater Rinse
Until you can get to the dental expert, among the very best things you can do is swish warm, salty water around in your mouth. A good mix is 1/2 teaspoon table salt to 8 ounces of water. Spit it out, do not swallow it. You can likewise carefully floss around the aching tooth to remove any little bits of food that might be stuck.
OTC Pain Relievers
Dental experts recommend acetaminophen for children. For adults, take your pick of over-the-counter medicines, like ibuprofen to deal with extreme toothache. If you select aspirin, swallow it — do not put it right on the tooth or your gums! That folk solution doesn’t work and might harm the within your mouth.
Cold Compress
If your face is swollen, put an ice pack on your cheek. It might assist ease the pain, especially if you’ve chipped your chopper or knocked it loose. Swelling might likewise indicate you have an abscess, a sac of pus and gunk deep in the roots of your tooth. This can cause serious infection in your jaw and other teeth. Signs consist of fever and red gums.
OTC Anesthetics
Apply these pain-relieving gels and liquids directly to the aching tooth and nearby gums. They contain benzocaine, which will numb your mouth for a little while. Be careful: They’re indicated for short-term use only and you extreme tooth pain may return in the next few hours.
Ice
Put some ice in your hand, on the same side of the body as your sore tooth. Rub the ice in the space in between your thumb and forefinger for 7 minutes, or till the area turns numb. Why does it work? Scientists believe ice stops pain signals to your brain.
Clove Oil
This natural solution numbs pain. Rub it directly on the aching area, or soak a cotton ball and dab it against the tooth and gums. It might be as effective as benzocaine, the numbing active ingredient in non-prescription toothache gels.
Garlic
When you squash one of these cloves, you launch allicin, an oily liquid, and natural disease fighter. Will it reduce the ache? That’s unclear. However, you can attempt chewing a piece of garlic, or placing sliced bits on your tooth. It’s safe — other than, of course, for your breath.
Toothache Plant
With a name like that, this might seem a sure bet to reduce your symptoms. Various types of this plant growing all over the world and the oil is an ingredient in many products. But it’s not yet clear if this plant truly works to ease oral pain.
Conclusion
The best thing you can do if faced with extreme tooth pain is to contact your dentist as soon as possible. If this is not possible in the near future, the best solution for such pain will certainly be strong painkillers listed in the article. However, if it happens that they are not at hand, the proposed methods of home remedy will be useful until you get to a doctor who can provide you with qualified assistance.