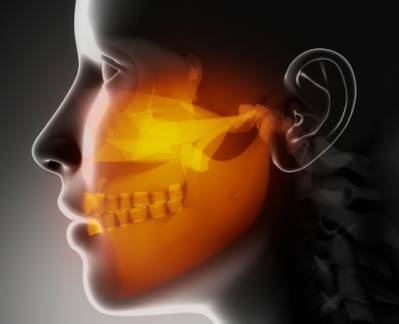
Temporomandibular Joint disorder (TMJ) is a problem impacting the ‘chewing’ muscles and the joints in between the lower jaw and the base of the skull. Medical professionals in some cases describe the condition as “myofascial pain disorder”.
It’s been approximated that approximately 30% of adults will experience TMJ at some time in their lives.
The condition itself isn’t really generally severe, and the symptoms it can cause – consisting of pain, jaw joint clicking or popping, and problems consuming – typically just last a couple of months before improving.
Pro Tip: This Portable Water Flosser is up to 50% more effective than traditional floss and can save you hundreds on professional dental cleanings. Its 300ml tank and cordless design make it perfect for maintaining healthy gums. Check the current deal on Amazon.
Nevertheless, these symptoms can substantially lower quality of life, and professional treatment may be needed if they’re severe.
Temporomandibular Joint Disorder Symptoms
TMJ can cause:
- clicking, popping or grating noises as you chew or move your mouth
- muscle pain around the jaw
- pain in front of the ear that might spread to the cheek, ear and temple
- problem opening the mouth– the jaw may feel tight, as if it is stuck, making eating difficult
- headache or migraine
- earache or a “buzzing” or obstructed experience in the ear
- pain in other areas of the body– such as neckache or backache
These symptoms may result in associated symptoms, such as disturbed sleep.
What Causes Temporomandibular Joint Disorders?
Possible causes of TMJ include:
Dental Care: This Rotating Electric Toothbrush removes up to 400% more plaque than a manual brush. With a built-in pressure sensor and 8 replacement heads included (a 2-year supply), it’s a cost-effective way to maintain a professional clean at home. Available on Amazon.
- clenching your jaw or grinding your teeth during sleep (bruxism) – which exhausts the jaw muscles and puts pressure on the joint (often caused by stress).
- wear and tear of the inside of the jaw joint — generally brought on by osteoarthritis.
- injury to the jaw joint — for example, after a blow to the face or surgery.
- stress — some individuals might acquire increased level of sensitivity to pain or stress.
- unequal bite — for example, when brand-new fillings, dental crowns or dentures are fitted.
- specific diseases — TMJ might be connected with specific illness such as rheumatoid arthritis, gout or fibromyalgia.
However, some people might develop TMJ without an obvious cause being discovered.
How Long Do TMJ Symptoms and Signs Last?
- Acute TMJ symptoms and signs might last anywhere from a couple of days to a couple of weeks and after that vanish after the injury or cause of discomfort has solved.
- For a chronic TMJ condition, the symptoms can be ongoing with episodes of sharp and/or dull pain that happen over an extended amount of time (months to years).
What Are Risk Factors for TMJ Disorders?
Ongoing studies carried out by the National Institute of Dental and Craniofacial Research (NIDCR), part of the U.S. National Institutes of Health, are focused on examining threat aspects for TMJ syndrome in healthy individuals. Preliminary outcomes have actually determined a group of physiological, psychological, sensory, and genetic and nerve system factors that may increase the danger of establishing TMJ syndrome. New findings will allow us to much better comprehend the start and development of TMJ syndrome. In addition, novel methods to detect and deal with the condition can be established. Below are some threat aspects that have been recognized:
Gender: Women are at higher danger of establishing TMJ syndrome compared to men. Additionally, there might be differences in how women and men react to pain and to pain medications.
Age: Studies of people in between the ages of 18-44 show that the danger to develop TMJ conditions boosts for women. This has actually been noted specifically for women during their childbearing years. For men ages 18-44, there was no increased danger.
Pain tolerance: Studies recommend that individuals who are more conscious slightly painful stimuli have actually an increased risk of developing TMJ syndrome.
Genes: There is some indicator that genes connected to stress reaction, mental health, and inflammation might increase the danger for TMJ syndrome.
Chronic pain: Those who struggle with chronic pain conditions such as lower back pain and headaches might be at increased threat for TMJ syndrome.
TMJ Disorders Treatment
If you have TMJ, see your GP or dental professional first for medical diagnosis and to discuss treatment choices.
Generally, non-surgical treatments such as lifestyle changes and self-help physiotherapy-type treatments are tried first.
A small number of people with severe TMJ may be described an oral and maxillofacial surgeon to discuss further treatment alternatives.
Lifestyle changes
There are a variety of self-help steps that can assist improve TMD, including:
- resting the joint by eating soft food and avoiding chewing gum.
- holding a warm or cold flannel to the jaw for 10-20 minutes, numerous times a day.
- doing a few gentle jaw-stretching exercises– your health care specialist can recommend proper exercises.
- preventing opening the joint too broad up until the pain settles.
- preventing clenching the teeth for long periods of time.
- massaging the muscles around the joint.
- relaxation techniques to alleviate stress.
- not resting your chin on your hand.
Mouth guards
Mouth guards (plastic devices that fit over your teeth) may be valuable if you grind your teeth. These cover the teeth during the night to lower jaw clenching and teeth grinding, and can be made to determine by your dental practitioner.
Medication
Painkillers such as paracetamol, ibuprofen or codeine can help alleviate the pain associated with TMD. If these aren’t enough to manage the pain, your doctor might prescribe more powerful medication such as a muscle relaxant or antidepressant. (More information regarding medications for TMJ see below.)
Steroid injections
If TMJ is caused by a disease such as arthritis, a steroid injection into the jaw joint can help in reducing pain and swelling in a joint or the surrounding soft tissue. The majority of people report feeling less pain within the first 24 hours to one week. You might find your pain enhances for a duration of a few weeks to a number of months and, in some cases, the injection solves the pain entirely.
Surgery
If the above procedures do not help and the source of your symptoms is the temporomandibular joint– rather than the chewing muscles– your expert might recommend a surgical treatment such as arthrocentesis (joint wash-out). Open joint surgery may be thought about in the rare cases where there is a problem within the joint. Overall joint replacement might be recommended for an exceptionally little number of people with severe, lasting symptoms and impaired jaw function. The National Institute for Health and Care Quality (NICE) has actually produced guidelines on this procedure. All joint surgery can have substantial side effects and you need to talk about these with your cosmetic surgeon.
Outlook
A lot of cases of TMD enhance over time and do not worsen, and many people will not need surgery. In the meantime, symptoms can typically be improved with the treatments discussed above. Although not a severe condition, temporomandibular condition can make a considerable effect on lifestyle.
Medications Used for TMJ
Medications are handy just for symptomatic relief and should be used only for short periods. NSAIDs, whenever used, ought to be administered on a short-term regular basis and not prn.
Nonsteroidal anti-inflammatory agents (NSAIDS)
Class Summary: These agents have analgesic, anti-inflammatory, and antipyretic activities. Their mechanism of action is not known, but they might inhibit cyclooxygenase activity and prostaglandin synthesis. Other systems might exist as well, such as inhibition of leukotriene synthesis, lysosomal enzyme release, lipoxygenase activity, neutrophil aggregation, and various cell-membrane functions.
Ibuprofen (Motrin, Ibuprin)
DOC for mild to reasonably serious pain; inhibits inflammatory responses and pain by reducing prostaglandin synthesis.
Naproxen (Aleve, Naprelan, Naprosyn)
For relief of mild to reasonably extreme pain; hinders inflammatory responses and pain by decreasing activity of cyclooxygenase, which is responsible for prostaglandin synthesis.
Muscle relaxant
Class Summary: These agents ease muscle spasms.
Methocarbamol (Robaxin)
Decreases nerve impulse transmission from spinal cord to skeletal muscle.
Cyclobenzaprine (Flexeril)
Skeletal muscle relaxant that acts centrally and minimizes motor activity of tonic somatic origins, affecting both alpha and gamma motor nerve cells. Structurally related to tricyclic antidepressants; for that reason, has a few of very same restrictions.
Benzodiazepines
Class Summary: By binding to particular receptor sites, these agents appear to potentiate the impacts of GABA and help with repressive GABA neurotransmission and other inhibitory transmitters.
Diazepam (Valium, Diastat)
- Depresses all levels of CNS (eg, limbic and reticular formation), perhaps by increasing activity of GABA.
- Individualize dosage and boost carefully to avoid adverse effects.
- Neuromuscular Blocker Agent, Toxin.
- Class Summary: Utilized experimentally.
Botulinum contaminant type A (BOTOX)
One of numerous contaminants produced by Clostridium botulinum. Blocks neuromuscular transmission through a 3-step process, as follows:.
- blockade of neuromuscular transmission; botulinum contaminant type A (BTA) binds to the motor nerve terminal. The binding domain of the type A particle seems the heavy chain, which is selective for cholinergic nerve terminals.
- BTA is internalized via receptor-mediated endocytosis, a process in which the plasma membrane of the afferent neuron invaginates around the toxin-receptor complex, forming a toxin-containing vesicle inside the nerve terminal. After internalization, the light chain of the contaminant particle, which has been demonstrated to include the transmission-blocking domain, is released into the cytoplasm of the nerve terminal.
- BTA blocks acetylcholine release by cleaving SNAP-25, a cytoplasmic protein that is located on the cell membrane and that is needed for the release of this transmitter.
The impacted terminals are inhibited from stimulating muscle contraction. Toxic substance does not affect synthesis or storage of acetylcholine or conduction of electrical signals along the nerve fiber. Usually, a 24-72 h delay between administration of contaminant and beginning of clinical effects exists, which terminate in 2-6 mo. This cleansed neurotoxin complex is a vacuum-dried type of purified BTA, which contains 5 ng of neurotoxin complex protein per 100 U.
Treats excessive, unusual contractions associated with blepharospasm. BTA has to be reconstituted with 2 mL of 0.9% sodium chloride diluent. With this solution, each 0.1 mL results in 5 U dosage. Client needs to receive 5-10 injections per visit. Need to be reconstituted from vacuum-dried toxin into 0.9% sterilized saline without preservative using manufacturer’s instructions to provide injection volume of 0.1 mL; need to be utilized within 4 h of storage in fridge at 2-8 ° C. Preconstituted dry powder need to be saved in freezer at less than 5 ° C.
Reexamine patient 7-14 d after initial dose to evaluate for action. Increase doses 2-fold over previous one for patients experiencing incomplete paralysis of target muscle. Do not go beyond 25 U when offering it as single injection or 200 U as cumulative dose in 30-d period. For the purpose of TMD treatment, studies are restricted and the medication is not authorized.
TMJ Home Remedies: How to Help Yourself?
In the majority of cases, TMJ syndrome is self-limiting. Most of the symptoms vanish in 2 weeks as soon as the jaw is rested There are a range of options for treating TMJ syndrome at home.
- Anti-inflammatory and pain medications such as aspirin or acetaminophen (Tylenol) or ibuprofen (Motrin, Advil) may offer relief.
- Eat a diet of soft foods.
- Avoid chewing gum and eating tough candy or chewy foods. Do not open your mouth wide. Your doctor may show you how to perform mild muscle extending and relaxation exercises.
- Stress-reduction strategies might help you handle stress and relax your jaw together with the rest of your body.
- Apply warm compresses on the area of pain. Home treatment consists of mandible (lower jaw) movements, such as opening and closing the jaw from side to side. Try this after a warm compress is looked for 20 minutes. The lower jaw motions should be duplicated 3 to 5 times a day, five minutes continually each time, for about two to four weeks. A mild massage of the area can also be beneficial.
What type of doctor should I see for TMJ?
Haveing a TMJ problem, what type of doctor do I consult with?
Answer
The temporo mandibular joint, or TMJ, is as you understand the joint where the lower jaw bone connects to the skull. Temporo mandibular joint pain syndrome is a very common medical issue, and symptoms usually include pain in the joint, particularly with chewing. There may likewise be difficulty opening the mouth large in more severe cases.
TMJ pain syndrome is frequently picked up and examined initially by your dental practitioner. Therefore, this would be a good location to begin for an assessment, if you have not seen any medical professionals yet at all. The reason that dentists are so involved in the treatment of TMJ pain syndrome is that the majority of the causes of the problem related to the mechanics of the teeth and the jaw. For example, over biting in the mouth or misalignment of the teeth of the upper and lower jaw is the most common cause of TMJ pain. Similarly, grinding of the teeth, which usually takes place at night, is also related to TMJ pain. Your dental professional will have the ability to evaluate you for these causes and, if they discover something, they will be able to recommend various treatments, which could include anti inflammatory medications, physical therapy, or bite guards. Please see your dental practitioners soon.
Prevention Steps
- If you tend to have occasional bouts of jaw pain, prevent chewing gum or biting on items, such as pens or fingernails. Avoid consuming hard or chewy food. When you yawn, support your lower jaw with your hand.
- Prevent big bites while consuming.
- Regularly massage your jaw, cheeks and temple muscles.
- If you feel spasms, apply damp heat.
- Keep good sleep posture with neck assistance.
- Avoid nestling the phone between your shoulder and neck.
- See your dental practitioner if you grind your teeth at night or discover yourself clenching your jaw. The dental expert can make a splint for you.
Prognosis of TMJ
Many people do well with conservative therapy, such as resting the jaw or utilizing a mouth splint. The success of treatment depends upon how extreme the symptoms are and how well you comply with treatment.
Only about 1% of those with TMJ syndrome require joint replacement surgery.