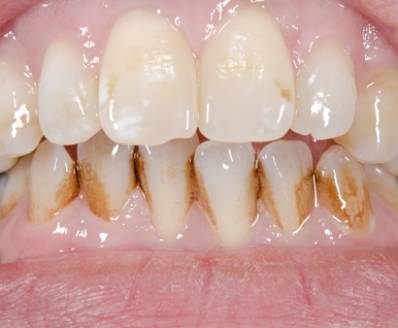
There are numerous scenarios that can cause discolored teeth. The majority of the time, the discolorations are “extrinsic,” impacting the tooth enamel alone, and can be fixed.
What Causes Teeth Discoloration?
An example of extrinsic discoloration is stains triggered by foods or beverages. Black tea or coffee; and darkly colored foods such as beets or chocolate are prime culprits. Other foods likely to stain teeth are berries, popsicles, sweets and pickles.
Soy sauce, curries and tomato sauce can cause teeth to yellow with time, and smoking cigarettes and other tobacco can stain teeth as well. In addition, producing an acidic environment in the mouth, whether through eating acidic food or by not brushing and flossing routinely, can make the enamel more vulnerable to staining.
Pro Tip: This Portable Water Flosser is up to 50% more effective than traditional floss and can save you hundreds on professional dental cleanings. Its 300ml tank and cordless design make it perfect for maintaining healthy gums. Check the current deal on Amazon.
There are 3 primary types of tooth discoloration:
- Extrinsic – This happens when the outer layer of the tooth (the enamel) is stained. Coffee, soda or other beverages or foods can stain teeth. Smoking cigarettes also causes extrinsic stains.
- Intrinsic – This is when the inner structure of the tooth (the dentin) darkens or gets a yellow tint. You can get this type of staining if:
- You had excessive exposure to fluoride during early youth.
- Your mother used tetracycline antibiotics during the second half of pregnancy.
- You used tetracycline antibiotics when you were 8 years old or more youthful.
- You had trauma that impacted a tooth when you were a young child. A fall, for example, might harm the establishing long-term tooth.
- You had injury in an irreversible tooth, and internal bleeding discolored the tooth.
- You were born with a rare condition called dentinogenesis imperfecta. This causes gray, amber or purple stainings.
- Age-related – This is a mix of extrinsic and intrinsic elements. Dentin naturally yellows over time. The enamel that covers the teeth gets thinner with age, which allows the dentin to show through. Foods and smoking likewise can stain teeth as people age. Finally, chips or other injuries can blemish a tooth, specifically when the pulp has been harmed.
Real examples of why teeth darken and change color:
- Green-blue or brown staining of temporary teeth seen in children who have had hemolytic jaundice in infancy. These stains are the result of postnatal staining of dentin with bilirubin and biliverdin.
- Characteristic brown staining of teeth caused by destruction of a large number of red blood cells in fetal erythoblastosis as a consequence of fetal rhesus maternal incompatibility.
- Red-brown staining of the teeth in persons suffering from porphyria, a very rare disease in which excessive amounts of pigment are produced.
- Changes in the color, shape and structure of the teeth almost inevitably occur with aging. The nature and extent of these changes depend on a combination of genetic factors, lifestyle and various bad habits. Years of smoking and coffee consumption have a cumulative staining effect. These and other types of pigmented plaque become even more prominent due to the inevitable formation of cracks and other changes in the tooth surface within its crystalline structure, in the underlying dentin and pulp. In addition to tooth abrasion and trauma, old amalgam fillings and other restorations may begin to deteriorate. Even with very careful attention to these problems, teeth will change color as they age due to natural abrasion as well as exposure to the oral environment. Initially, there is usually a thinning of the enamel. In this process, the cheek surface of the tooth becomes flatter and there is a gradual discoloration of the tooth due to the loss of the clear enamel layer. As the enamel thins, secondary dentin begins to form through a natural defense mechanism in the dentin and pulp. This increased mass of dentin begins to darken. Thin enamel combined with darkened dentin gives the teeth an “older” appearance.
- White stains symmetrically placed on the same teeth can be a symptom of enamel hypoplasia. One of the features of hypoplasia stains is that they are not stained with dyes, and the outer layer of enamel remains smooth, shiny. Chalky teeth can be a consequence of excessive bleaching, the long-term use of soda for this purpose. Small chalky stripes – strokes located in the sub surface layers of enamel are characteristic of the streaky form of fluorosis. The spotted form of fluorosis is characterized by chalky spots without stripes. The chalky form of fluorosis is characterized by a considerable variety. Usually the enamel of teeth has a matte shade, and against this background, pigmented spots with clear boundaries are visible. Sometimes a large number of spots and dots are found on the enamel. The pronounced whitish color may be due to dense plaque that has formed due to inadequate or improper individual oral hygiene.
- Dentures that have been pulped lose their distinctive shine and take on a more grayish hue. A similar, and sometimes more intense color change is seen in teeth with pulp necrosis. Gray staining can also be caused by heavy metal poisoning – mercury and lead.
- Teeth with a greenish tint appear when their surface is affected by specific fungi. Green staining can occur when a tooth comes into contact with copper amalgam fillings. Yellow teeth can result from exposure to bromine and iodine fumes, as well as the constant consumption of strong tea and coffee. A dark brown fringe often appears in smokers. Dark brown (up to black) tooth color can occur with occupational exposure to metals (manganese, iron, nickel). Tooth crown discoloration can occur immediately after an injury, especially in the cervical area on the palatine side where the enamel layer is thinner, which is a diagnostic sign of trauma. Thus, tooth discoloration clinically manifests itself in a wide variety of shades.
To summarize, let’s highlight the main causes of tooth discoloration:
There are many external and internal causes of dental unit discoloration. Among the most common are the following:
- Consumption of colorful foods: coffee, tea, carbonated drinks, dark berries. The color pigments gradually penetrate the enamel, which leads to its darkening.
- Smoking: Resins from tobacco get deposited on the tooth surface and form a hard-to-remove film.
- Inadequate oral hygiene: Not only do you need a professional toothbrush and toothpaste to clean plaque, but you should also floss and use an interdental brush. Many people neglect these tools, resulting in the formation of tartar that disrupts the natural color of the enamel.
- Systemic diseases affecting the teeth: Certain pathological conditions (e.g., a metabolic disorder) can cause discoloration or “darkening” of the dentin.
- Genetic predisposition: People differ in the thickness and density of their enamel. The thicker it is, the less influence external factors have on its color.
- Medications: Certain medications change the color of your teeth. These include antidepressants, antihistamines, and blood pressure pills. Childhood use of tetracycline antibiotics also leads to discoloritis.
- Natural age-related changes: Enamel gradually wears away, exposing yellow dentin, which affects the color of the units. In addition, the teeth have more and more deposits, stains, their structure changes, which leads to a darkening of the hard shell.
- Environmental influence: Continuous use of fluoride-containing substances also has a negative effect on the natural whiteness of dental units. Fluoride levels are often elevated in drinking water, and some foods may also accumulate fluoride.
- Certain medical procedures, such as chemotherapy, can change the natural color of your teeth.
- Damage to the dental nerves: trauma or unsuccessful surgical procedures that result in damage to the nerve tissue can also be a cause of discoloration.
The dentist determines the exact cause of the discoloration of the dental tissues and recommends the best technology to eliminate dark or whitish stains.
Dental Care: This Rotating Electric Toothbrush removes up to 400% more plaque than a manual brush. With a built-in pressure sensor and 8 replacement heads included (a 2-year supply), it’s a cost-effective way to maintain a professional clean at home. Available on Amazon.
Influence of oral diseases on tooth enamel color changes
Certain pathologies lead to discolorations, and the color will depend on the type of disease:
- Teeth turn gray when nerve tissue is destroyed and/or the pulp is removed. Another cause is heavy metal poisoning. Whitening and grinding only partially removes the visual defect, most often dentists recommend placing veneers.
- The tooth surface becomes pink with the treatment of root canals with a resorcinol-formalin mixture. Chronic diseases of the pulp and periodontium also lead to redness of tissues. Cases of typhoid, cholera, porphyria and rheumatism have been reported to cause discoloration of dentin.
- Blue color indicates alkaptonuria, a genetic disease associated with a metabolic disorder in the body.
Changing the color of the tooth in systemic diseases is associated with a violation of the normal composition of dentin. It darkens (turns red or loses its pigment) and begins to show through the clear enamel. This is an internal cause of discoloration, and classical bleaching is not enough to eliminate it.
In some cases, experts recommend intracanal restorations. The technique involves applying a whitening compound outside and inside the unit, so the effect is not only on the enamel, but also on the dentin. However, endodontic whitening is only suitable for pulpy teeth.
Symptoms of Teeth Discoloration
Symptoms include discolorations on the enamel. They can range from white streaks to yellow tints or brown spots and pits. If the enamel has actually worn away, and dentin is showing through, you may discover a yellow tint.
Diagnosis
No special tests are needed. A dental professional or other dental professional can detect tooth discoloration by looking at the teeth.
Expected Duration
Some teeth discoloration can be gotten rid of with professional cleansing. An example would be the discolorations triggered by coffee. Many stains are irreversible, however. Teeth sometimes can be whitened with a lightening gel. Sometimes, if the staining is severe, a crown or veneer may be required to cover it.
Indications for teeth whitening
- The patient’s desire to make their teeth lighter.
- A mild to moderate form of fluorosis.
- Age-related discoloration of the teeth (yellowing).
- Staining due to bad habits.
- Penetrating staining from frequent consumption of colorful foods and beverages.
Contraindications
General
- Age of the patient (underage children and adolescents).
- Pregnancy and breastfeeding.
- Allergic reactions to bleaching components.
- Taking photosensitive drugs such as doxycycline, tretinoin, ciprovloxacin, hydrochlorothiazide, etc.
- General diseases: cancer and endocrine disorders, bronchial asthma, hypertension.
- Excessive expectations of the patient from the whitening procedure.
Local
- The presence of cavities, fillings, restorations, crowns in the whitening area.
- A wide pulp cavity.
- Hyperaesthesia of enamel (increased tooth sensitivity).
- Significant loss of enamel due to pathological and age-related.
- Acute and exacerbated periodontal disease.
- Diseases of the mucous membrane of the mouth.
- Diseases of the temporomandibular joint accompanied by limitation of mouth opening.
- The presence of a pronounced gag reflex in the patient.
Teeth Discoloration Prevention
Brushing your teeth after every meal will help to prevent some spots. Dental professionals suggest that you wash your mouth with water after having coffee or other beverages or foods that can stain your teeth. Regular cleansing by a dental hygienist also will help to remove surface area discolorations.
Intrinsic discolorations that are caused by damage to a nerve or blood vessel in a tooth in some cases can be avoided. You might have to have root canal treatment to get rid of the inner part of the tooth (the pulp) before it has an opportunity to decay and darken. However, teeth that have root canal treatment might darken anyhow.
To prevent intrinsic spots in children, prevent excessive early direct exposure to fluorides. Once the enamel is formed, fluoride will not discolor teeth.
Treatment for Teeth Discoloration
Many extrinsic spots triggered by food and drink can be gotten rid of by regular expert cleanings and home care. Great home care includes brushing, flossing and rinsing after meals.
Discoloration often can be removed by applying a lightening representative to the tooth enamel. One strategy is called “power whitening.” With this technique, the dentist applies a light-activated lightening gel. It causes the teeth to obtain substantially whiter in about 30 to 45 minutes. Several follow-up treatments may be required, or take-home lightening trays might be provided.
It’s likewise possible to remove staining at home. You will use a whitening gel and a mouth guard given to you by your dentist. The bleaching gels developed for use at home aren’t as strong as those used by your dental professional. This suggests that the procedure takes longer– typically two to four weeks.
You also can buy whitening products nonprescription. They include a weaker bleach than the products you can obtain from your dentist. The whitening representative is applied as a gel put in a mouth piece or as a strip that stays with your teeth. Over the counter mouth pieces fit less safely than the kind you receive from your dental professional, however they will lighten your teeth gradually.
Bleaching tooth pastes may remove minor stains. They do not in fact alter the overall color of your teeth.
If your tooth has darkened after a root canal, whitening the enamel will not help. Your dental expert can apply a whitening material to the inside of the tooth, or you might consider a crown or veneer.
Lightening will not lighten some stains, such as tetracycline discolorations. In this case, your dental professional might recommend covering the tarnished areas. This also might be useful when the tooth is chipped or severely damaged.
A tooth can be covered with a color-matched composite bonding material. Another option is to get veneers. These are thin ceramic shells that cover the outer surfaces of the teeth.
Possible complications
- Appearance of hyperesthesia (can last from several hours to several days). To eliminate it, it is necessary to carry out a course of remedial therapy before and after the whitening procedure. The use of desinitizers, special rinses and pastes for sensitive teeth.
- Irritation of the oral mucosa (burning).
- Color regression. Within 2 weeks after the bleaching procedure, the oxidation process changes the optical qualities of the tooth, giving it a more opaque appearance. After 2 weeks, the oxygen dissipates and the tooth takes on a real lighter shade.
- A change in taste sensation. This is temporary in nature.
In order to maintain the results, the patient must observe the following recommendations
- Daily observance of the rules of individual oral hygiene.
- In the first 48 hours after bleaching procedures, do not eat any colorful food, and in the next 2 weeks, follow a transparent diet.
- Regularly visit the dentist at least once every six months.
- The repeated course of bleaching in 1.5-2 years (if necessary).
Teeth whitening procedure scheme
- Questionnaire
- Collecting medical history
- Determining the cause of discolouration of teeth
- Indications and contraindications.
- Discussion of complications and side effects after the teeth whitening procedure.
- Discussion of patient behavior after the course of whitening.
- Drawing up a patient’s informed voluntary consent to the whitening procedure.
- Determination of the original color of the teeth by Vita+photomicrographs.
- Professional oral hygiene.
- Application of a protective gel to the mucous membrane.
- Applying a whitening gel to the teeth (3 sessions of 15 minutes)
- Registration of the results (color according to the Vita scale + pictures, presence of complications)
- Conducting a course of remedial therapy after the whitening procedure.
- Recommendations after bleaching procedures, individual selection of oral hygiene products, appointment of a date for a follow-up examination.
- Re-examination. Determining the need for a second course of whitening. In order to maintain consistency of the results – prescription of home tooth whitening products (if necessary)
- Repeated whitening procedure (if necessary).
Ways to restore your teeth to their natural whiteness
The whitening technique depends on the cause of the discoloration. For example, when taking tetracycline antibiotics, teeth take on an unattractive blue-gray or yellow-brown color. Because this is caused by structural changes in the tissues, it is not possible to remove this defect with regular bleaching. The optimal solution is porcelain veneers, which effectively compensate for any aesthetic imperfections in the tooth.
Another common reason for tooth discoloration is the excessive use of fluoride-containing products during the period of tissue formation (fluorosis). Under its influence, brown areas and/or chalky-white spots and stripes appear on the teeth. In this case, combined methods are used. For example, finely abrasive whitening is carried out. The procedure involves the application of a special paste containing a fine abrasive. With the help of polishing particles, darkened areas are polished. At the same time, the safe acid included in the composition eliminates decalcification and gets rid of unsightly whitish stains on the teeth.
But most often, dentists are faced with discoloration caused by regular consumption of colorful foods, drinks and smoking. The pigments gradually accumulate and appear as yellow, brown, green and orange stains on the enamel. These kinds of stains are removed by deep cleaning. But it is even easier to prevent staining of the teeth. To do this, it is enough to observe oral hygiene.
If the enamel has already changed color, the classical whitening technology based on the use of hydrogen peroxide will help to correct the situation. Such compositions are safe, do not affect the structure of hard tissues and significantly lighten the tone of the teeth.
Effectiveness of bleaching for discolorations
Bleaching gives the best results with external discoloration: for example, in the case of staining of tooth enamel with food dyes. But the procedure is not always effective. Technology to restore the aesthetics of the teeth must be chosen based on the cause of the darkened tissue.
For example, if teeth are losing their whiteness due to natural aging, a one-time whitening treatment will not produce a noticeable result. Regular visits to the dentist’s office at intervals recommended by a professional are necessary.
It is more difficult to restore the beauty of a smile with congenital color anomalies. In these cases, neither grinding nor chemical whitening is able to achieve an attractive shade. If the aesthetic defect causes the patient serious psychological discomfort, the best solution is to have veneers placed.
It is also recommended to combine bleaching with other methods to restore the color of teeth in the following cases:
- Destruction of the teeth. Caries and necrosis leads to a gradual change in the shade of tissue. To stop the pathological process, it is necessary to carry out a comprehensive treatment, to install fillings and dentures. After that, whitening can be performed, if necessary.
- Use of poor quality dental materials. Defective or old dentures gradually deteriorate and stain the surrounding tissues black, brown and gray. Over time, metal fillings that show through translucent enamel may become darker. Bleaching does not change the color of the artificial materials and will not protect your teeth from further staining. The first step is to eliminate the source of discoloration by placing modern dentures.
- Complicated dental treatment or trauma to the maxillary tissues. In some cases, the restoration of dental canals in the late stages of disease leads to discoloration of the hard tissues: they turn gray, the tooth loses its whiteness and stands out against its “neighbors”. This is an internal reason why whitening must be combined with other techniques to restore aesthetics. If the unit darkens without external damage – most often it indicates the death of nerve tissue. In this case it is necessary to first treat the tooth and only then think about bleaching or a crown.
Bleaching is also not suitable if there is a systemic disease affecting the dental tissue. However, this does not mean that you have to forget about the white-toothed smile.
Toothpastes with a whitening effect
Patients often ask: Is whitening toothpaste enough to whiten my teeth?
The main purpose of whitening toothpastes is to maintain the results achieved by professional whitening.
The whitening ingredients in toothpastes:
- Substances that dissolve plaque (proteolytic enzymes: bromelain, papain)
- Substances with an increased cleansing effect (sodium bicarbonate)
- Plaque inhibitors (xylitol, bromelain, triclosan and copolymer).
- Substances that inhibit plaque mineralization (pyrophosphates, zinc citrate).
When deciding to use toothpastes with a whitening effect, there are a number of things to consider: Polishing abrasive toothpastes are very common on the market. Continuous use of such pastes leads to abrasion of tooth enamel, so such pastes are not recommended as regular. You can pick up different modes of their use. But such pastes are categorically not suitable for those who have cervical defects of teeth.
Sometimes the manufacturers of toothpastes promise to lighten the teeth by several tones. This effect is achieved with a toothpaste that contains carbomide peroxide, like home whitening systems. At the same time, the concentration of carbomide peroxide should be 8-10 percent. The main distinguishing feature of such toothpaste is its specific peroxide taste. These pastes are technologically very difficult to produce, so the offerings on the market are few.
When To Call a Professional
Tooth staining is mainly a cosmetic problem. Check out a dental practitioner if you’re unhappy with how your teeth look. Any change in a child’s normal tooth color need to be assessed by a dental expert.
Conclusion
Teeth color is affected by many factors, but we can identify two key reasons that lead to a change in shade: either the enamel is damaged (thinning, plaque accumulation), or there is a structural change in dentin caused by dental disease or systemic pathology. In the first case, traditional bleaching gives a good result: the dentist gently cleanses the enamel from plaque and calculus, and uses special formulas that return it to its natural whiteness.
If the discoloration of the teeth is due to internal reasons, external action is not very effective. The optimal choice is to install veneers, which will hide any external defects, including chips and tooth surface irregularities. In any case, a professional dentist can help restore a whiter smile.