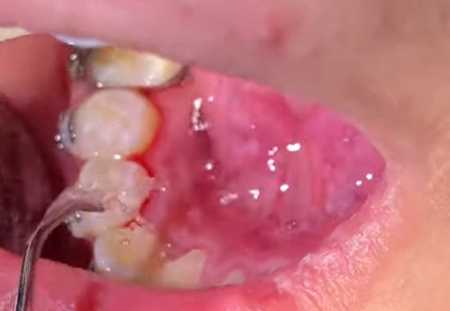
A common question on various forums is “what should I do if my gum is swollen or there is swelling near my tooth”? There may be different accompanying symptoms: there may or may not be pain in the gum; there may or may not be a fistula; the tooth may hurt, the gum may bleed, and there may be many other symptoms. Treatment for swollen gum in Samara depends directly on what the cause of the swelling on the gum was.
In this article, we will try to figure out what can cause a swollen gum, what symptoms other than swelling can help determine the cause of this swelling and what to do at home before you can go to the dentist.
Why Can the Gum Swell, Causes of Swelling
- Exacerbation of periodontitis;
- Exacerbation of chronic periodontitis or gingivitis;
- Abscess.
Of course, these are not all the possible causes of gum swelling, but about 90% of appeals (if not more) fall within this framework.
Pro Tip: This Portable Water Flosser is up to 50% more effective than traditional floss and can save you hundreds on professional dental cleanings. Its 300ml tank and cordless design make it perfect for maintaining healthy gums. Check the current deal on Amazon.
How to Treat Swollen Gums, How to Relieve Swelling
Before taking any action, it is necessary to determine the cause of the appearance of swelling (the appearance of swelling). This is important, since the tactics of treatment in each case will be different and the actions that are necessary in some cases may be the cause of deterioration in others.
Periodontitis
Symptoms
Periodontitis is an inflammatory process in the bone associated with the entry of infection into the root canals of the tooth and its further spread into the bone. In conditions of reduced immunity (caused by colds, seasonal cold weather, or severe general illness), the inflammation in the bone may progress from a chronic course to the acute stage, which is accompanied by an increase in the amount of pus. As a consequence, there is pain and swelling of the gum. Periodontitis may occur in a previously untreated tooth or in an already treated tooth with filled root canals (if somewhere the root canals were not properly cleaned, additional canals were not found).
In exacerbation of chronic periodontitis there may be the following symptoms (not necessarily all of them, there may be only some of them):
Dental Care: This Rotating Electric Toothbrush removes up to 400% more plaque than a manual brush. With a built-in pressure sensor and 8 replacement heads included (a 2-year supply), it’s a cost-effective way to maintain a professional clean at home. Available on Amazon.
- Swelling of the gum in the area of the causal tooth;
- Swelling is small at first, with time it increases, the mucosa becomes more “tense”, after some time a fistula may appear – a white blister on the background of the swelling. The fistula eventually opens, pus flows out and the swelling gradually decreases;
- pain when pressing on the gum with your finger and/or biting on the tooth;
- the affected tooth does not respond to cold, heat, sweets;
- a cavity in the tooth (or, if the tooth was previously treated, a large filling);
- possible increase in body temperature.
Pain and swelling in periodontitis are due to an accumulation of pus, as soon as the pus comes out (through the fistulous passage if untreated, or through the root canals if the patient went to the dentist), the pain goes away.
If the fistula has opened, the swelling has gone, and there is no more pain, it does not mean that the problem is solved. The inflammatory process in the bone is still there and it is necessary to see a dentist.
How periodontitis in the acute stage is treated
It is necessary to see a doctor to clarify the diagnosis. At the dentist you will be X-rayed to determine the localization of the inflammatory process and its size. Depending on the location and size of the inflammation, your dentist will offer you three options for further treatment:
- Conservative treatment – treatment of the tooth, which creates an outflow of pus through the root canals, followed by a filling.
- Surgical treatment – extraction of the tooth and cleaning of the hole.
- Combined treatment (if there is already a large swelling, but the tooth is planned to be saved) – treatment of the tooth and application of antiseptic under a temporary filling, and at the same visit a loosening incision is made, through which pus will escape.
The dentist decides which method will be used and in what case. The method of treatment depends on the localization and size of the process, the condition of the tooth, the further possible prospects for the restoration of the tooth, the general state of health and many other factors.
In parallel with each of these interventions may be prescribed procedures to be carried out at home:
- Gargling with a soda-salt solution (1 teaspoon of soda and salt per glass of water);
- taking antibiotics (most often lincomycin 0.5 grams 3 times a day – 5-7 days);
- anti-inflammatory drugs.
What to do before the patient can see a dentist?
- Under no circumstances warm the place of swelling (do not apply heat, do not smear with anything);
- saline rinses (the more often the better – about 10 times a day);
- anti-inflammatory drugs;
- Do not start taking antibiotics without a doctor’s prescription – you can achieve that the picture of the process will be blurred and the doctor will not be able to determine the correct treatment tactics in this case;
- Painkillers and anti-inflammatory drugs should not be mixed. If you choose one drug, you should not take other drugs at the same time – it can be dangerous for your health and even for your life.
Acute gingivitis
Causes
Gingivitis is an inflammation of the gums, periodontitis is an inflammation of the gums with the involvement of bone tissue. These processes occur only in the tissues surrounding the tooth, without affecting it. Gingivitis and periodontitis usually do not bother the teeth themselves (except in cases where there is a parallel course of gum disease and dental disease). There are many causes of gingivitis (most commonly tartar, untreated cavities, improperly placed fillings and orthopedic appliances, and bite problems). Gingivitis can be acute or exacerbated chronic, periodontitis most often has a chronic course with periods of exacerbation. Exacerbations can occur due to the following factors:
- Trauma to the gum with sharp objects (cuts, punctures with fish bones)
- Foreign bodies in the periodontal pockets (chipped tartar, bones, fibrous food)
- Acute respiratory infections, acute respiratory viral infections, and other systemic diseases,
- frequent exacerbations of gingivitis in diabetes, diseases associated with decreased immunity,
- Taking medications that reduce immunity (corticosteroids and others).
Symptoms
In the acute stage of gingivitis are observed:
- Pain and swelling of the gum near a group of teeth (localized gingivitis) or the entire jaw (generalized gingivitis);
- Painfulness when brushing the teeth and eating;
- bleeding of the gums at the slightest impact (brushing, eating hard food);
- The gum is red, sometimes livid;
- Reaction to hot foods is also possible;
- painfulness when putting pressure on the gum;
- The teeth are partially covered by swollen gum.
In periodontitis, these symptoms are similar and the difference will be that in gingivitis there are no radiological changes in the bone, while in periodontitis there will be a decrease in the height of the interdental septa and not a clear pattern. In periodontitis there is also exposing of the tooth roots, but in the acute stage, due to swelling, the roots may be closed by the soft tissues.
Treatment
Gingivitis and periodontitis should also be treated by a dentist.
In the office, the following measures are carried out:
- removal of hard and soft dental deposits (possibly with anesthesia), polishing the surface of the teeth and exposed roots;
- Correction of fillings, removal of traumatic elements of prosthetic constructions;
- removal of foreign bodies, if any;
- treatment of the oral cavity with antiseptic solutions;
- application of anti-inflammatory drugs under the dressing;
- in severe cases, flap surgery may be required – the separation of gum tissue, cleaning of teeth, roots, bone from the stone and affected tissues, followed by suturing.
Along with this, antibiotics, anti-inflammatory drugs, pain relievers, and antiseptic rinses may be prescribed.
Before there is an opportunity to visit the dentist, you can take these measures:
- Gargling with a soda-salt solution (1 teaspoon of soda and salt per glass of water) and antiseptic solutions (chlorhexidine, furacilin – as directed);
- Be sure to brush your teeth. Use anti-inflammatory pastes and pastes to relieve bleeding gums (paradontax, lacalut active, tebodont and others), preferably using a floss;
- Treatment of the gums with anti-inflammatory drugs (the most well-known is metragil denta) 3 times a day, after brushing and rinsing;
- if it hurts to brush teeth – you can treat the gum with an anesthetic before brushing (dentol and other products used for teething babies).
If after 2-3 days there is no improvement, it is necessary to consult a doctor, as gingivitis can progress to a chronic form or there may be a worsening of the situation – the formation of an abscess.
Periodontal abscess
An abscess is a limited area of inflammation characterized by an accumulation of pus under the gum. In fact, it is a pus-filled cavity that looks like a hemispherical mass on the gum. The size of the abscess can reach the size of a walnut.
Causes
The causes of periodontal abscess can vary, but the most common are:
- The release of pus from chronic periodontitis in the acute stage;
- accumulation of pus in periodontitis;
- Deep trauma from a foreign object, in which the infection penetrated deep into the tissue (puncture with a fish bone, which left a piece of bone in the gum, for example).
Symptoms
- A bulging, semicircular mass on the gum;
- pain on pressure, firm, tense tissue, fluctuation symptom (when pressing on the mass, you can feel the fluid inside)
- swelling of the surrounding tissues;
- The swelling may spread to the cheeks, resulting in facial asymmetry;
- An increase in body temperature may occur.
Treatment
Treatment of an abscess in Samara depends on the cause of its appearance. If it develops due to trauma (as in the case of the bone), the treatment is purely surgical – opening the abscess, removal of purulent contents, installation of drainage. If the cause is periodontitis or periodontitis, the treatment of the underlying disease is carried out in parallel.
After surgery, prescribe antibiotics, painkillers, anti-inflammatory, antihistamines, and after 3-4 days, when the swelling subsides and the drainage is removed, more and epithelializing drugs. This treatment is prescribed by the doctor.
Need to know:
- If you find symptoms similar to an abscess, you need to go to the doctor immediately. Delaying treatment can lead to the formation of phlegmon – a spilled inflammation, which usually ends in cuts on the outside of the face, and can also lead to sepsis – blood infection.
- Inflammatory processes should not be heated. When heated, microorganisms multiply more actively, and this can also lead to rapid progression of the process.
Other Diseases That Give Similar Symptoms
It has already been said above that 90% of patients’ complaints fall into one of the three cases already described. But that leaves another 10% who complain of “swollen gum.” Swelling or conditions similar in appearance can give pre-cancerous diseases, hormonal changes, cancer itself, HIV infection, diabetes and many other diseases. And with all there will be swelling, there will probably be pain. Therefore it is very important when you notice any swelling, overgrowths, bulges on the gum to consult a doctor to find out the cause of this phenomenon and timely treatment.