For all types of stomatitis lesions are treated with ointments, gels, sprays with a healing and antiseptic effect.
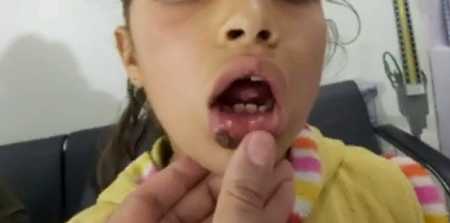
Stomatitis is an inflammation of the oral mucosa. Most often the pathology occurs in childhood and is accompanied by the formation of ulcers and wounds, which cause great discomfort to the patient. Pathogenic foci are localized on the tonsils, the inner sides of the lips and cheeks, as well as on the gums and under the tongue. The disease develops against a background of mechanical trauma, infections or dental disease.
If treated in time, the prognosis in all cases is favorable, so if you notice the first symptoms, see your doctor. Make an appointment at Left Bank Dental Clinic by phone, listed on the website or through the online form.
Pro Tip: This Portable Water Flosser is up to 50% more effective than traditional floss and can save you hundreds on professional dental cleanings. Its 300ml tank and cordless design make it perfect for maintaining healthy gums. Check the current deal on Amazon.
Types of Stomatitis
Depending on the cause that caused the development of the pathology, medical practice distinguishes between two types of stomatitis – infectious and non-infectious.
Also, the pathology is differentiated by type:
- Viral stomatitis – a consequence of infectious diseases or the impact of pathogenic microbes on the traumatized mucous membrane of the oral cavity. It appears as small blisters with a clear liquid, which gradually becomes cloudy. A painful ulcer is formed where the blister bursts.
- Fungal (candidiasis) – caused by the appearance of numerous ulcerous lesions covered with white plaque. It is caused by a fungus of the genus Candida.
- Radiation disease develops after the body has been exposed to ionizing radiation. It is accompanied by a significant thickening of the oral mucosa and the formation of painful erosions.
- Bacterial – most often caused by streptococcus or staphylococcus. Without treatment, it progresses rapidly, and numerous foci with purulent contents appear on the oral mucosa.
- Chemical – appears after burns of the soft tissues with any chemical substances. It appears as painful ulcers, which are mainly localized in the traumatized tissue.
- Aphthous stomatitis is the most common type of stomatitis, which develops due to a decrease in immune function, gastrointestinal diseases, and blood abnormalities. Painful ulcers about 5 mm in size affect the entire oral cavity, and without treatment very quickly spread and increase in size.
- Herpetic – develops due to infection of the body with herpes. Just as in the previous cases, sores are formed in the oral cavity, which cause considerable discomfort.
- Traumatic – occurs as a result of a single injury or due to constant exposure to damaging factors to the body (habit of chewing the lips, cracking nuts with the teeth, etc.). The main symptom is painful foci in the affected area.
- Mechanical – develops due to rubbing of the soft tissues with foreign elements – braces, dentures, plates for bite correction.
The risk group includes children under 7 years of age, elderly patients with internal diseases, patients who have lost several dental units, those who neglect personal hygiene, smokers and people with weakened immune system.
Important! All types of stomatitis without treatment not only rapidly affect the mucous membranes, but also spread to the internal organs. In neglected forms, diseases of the heart, blood and lungs develop, which is very dangerous for the life of the patient.
Dental Care: This Rotating Electric Toothbrush removes up to 400% more plaque than a manual brush. With a built-in pressure sensor and 8 replacement heads included (a 2-year supply), it’s a cost-effective way to maintain a professional clean at home. Available on Amazon.
Causes
The most common causes of the development of stomatitis include:
- Diseases of the gastrointestinal tract and oral cavity;
- The effects of chemotherapy;
- unbalanced and irregular diet;
- vitamin deficiencies in the body;
- trauma and burns of the mucous membranes of the mouth or gums;
- complications of pathologies of an oncological nature;
- hormonal imbalance;
- Abuse of alcoholic beverages and smoking;
- ingestion of pathogenic microorganisms on the traumatized oral mucous membranes;
- Various diseases occurring in a chronic form;
- Lack of oral hygiene or use of poor-quality toothpaste and brushes;
- Prolonged or incorrect use of any medications.
Another factor is unfavorable environmental conditions. Statistically, people who live in metropolitan areas get sick more often than those who live in places remote from the polluted cities.
Diagnosis
A visual examination of the patient is usually sufficient to make a diagnosis. If stomatitis is suspected to be the result of internal diseases, consultations with narrow specialists are prescribed.
If the disease is of infectious origin, the patient is referred for laboratory tests:
- oral smear to determine the type of pathogenic microorganisms;
- Blood tests to detect antibodies to internal organ pathogens;
- ELISA or PCR (polymerase chain reaction) – examination of biomaterial for detection of infectious agents.
If stomatitis is accompanied by a significant deterioration of health or increased body temperature, it is necessary to take general blood and urine tests. Diagnosis allows evaluating the general state of the body and identifying pathologies that have caused inflammatory processes in the oral cavity.
Methods of Treatment
If the pathology is of non-infectious origin, symptomatic treatment is carried out at home. For this purpose, decoctions and tinctures of medicinal herbs are often prescribed. With infectious stomatitis used medications aimed at eliminating the cause of the disease, and the removal of painful symptoms.
Treatment of Stomatitis in Children
Therapeutic measures vary depending on the type of pathology:
- Fungal stomatitis is treated with antiseptics and antifungal drugs. Rinsing of the mouth cavity is carried out at least five times a day.
- With herpetic stomatitis, irritating foods – spicy, sour, salty, fried, sweets, spices – are excluded from the diet. Of the medications used are immunostimulants, antiviral drugs, vitamin complexes and antiseptics for mouthwash. Since herpetic type is contagious, it is important to isolate the child with bed rest.
- Aphthous stomatitis is treated with antiseptics for irrigation and mouthwash, as well as vitamin complexes. In addition, all foods that can cause irritation to the mucous membranes of the mouth are excluded from the diet – citrus fruits, spices, chocolate, lemonade, potato chips, croutons and more.
- Bacterial stomatitis is treated with antibacterial medications and topical antiseptics.
- Chemical, traumatic and radiation types are treated with symptomatic treatment – painkillers, antipyretics and other drugs depending on the manifestations. The affected areas are also treated with antiseptics.
- Therapy of viral stomatitis involves taking antiviral drugs, immunostimulants and vitamin complexes.
For all types of stomatitis lesions are treated with ointments, gels, sprays with a healing and antiseptic effect. If local application means are not used, treatment can be significantly delayed.
Treatment in Adults
Therapy is carried out on the same principle as in children. If the causative agent of stomatitis is diseases of the internal organs, the patient is referred for consultation to the appropriate specialist, who will prescribe diagnosis and treatment.
Depending on the type of stomatitis, the following groups of drugs are used:
- antibiotics;
- antifungal;
- antiviral;
- anti-inflammatory;
- vitamin complexes;
- drugs to relieve painful symptoms – antihistamines, antipyretic, anti-edema and others.
To enhance the therapeutic effect of medications, it is recommended to give up products that irritate the mucous membranes, include dairy products in the daily diet, as well as fruits and vegetables (if not allergic).
Oral rinses are performed using ready-made pharmacy preparations or decoctions of herbs prepared at home. Most often the mucous membranes are irrigated using chamomile flowers, calendula, yarrow, sage or succession.
With timely access to the doctor’s prognosis in almost all cases is favorable, and complete recovery occurs after about 5-7 days. Advanced forms take much longer to heal.