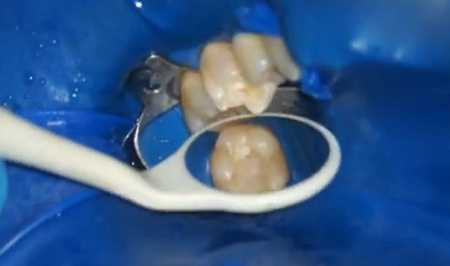
Pulpitis is an inflammation of the neurovascular bundle that fills the tooth cavity. Most often it develops due to caries, less often – due to improper manipulation by the doctor in the treatment of diseases of the gums or teeth.
The timely visit to a doctor is the guarantee of the rapid elimination of the pathology and preservation of the function of the tooth.
Classification of Pulpitis
The disease occurs in acute, chronic and aggravated chronic form. Acute pulpitis is accompanied by intolerable pain, with pain pills usually not helping. The pain syndrome usually covers a large area around the affected pulp, so the patient is not always able to specify exactly which tooth is bothering him.
Pro Tip: This Portable Water Flosser is up to 50% more effective than traditional floss and can save you hundreds on professional dental cleanings. Its 300ml tank and cordless design make it perfect for maintaining healthy gums. Check the current deal on Amazon.
Acute pulpitis is divided into three types according to the area affected:
- focal (partial);
- fibrous (total);
- purulent.
In the chronic form, purulent formations are localized not only in the area of the pathological focus, but also begin to penetrate deep into the gum. Often at this stage, the pain recedes, so a person thinks that the tooth has passed. This is far from being the case, and soon the inflammation makes itself felt again. In this case, the symptomatology is often even more serious than in the first exacerbation.
The condition is very dangerous to human health, so you should immediately contact a licensed dental clinic.
In addition to the fact that the disease is divided into forms, there are also types of pathology depending on the severity, size and area of the lesion.
Dental Care: This Rotating Electric Toothbrush removes up to 400% more plaque than a manual brush. With a built-in pressure sensor and 8 replacement heads included (a 2-year supply), it’s a cost-effective way to maintain a professional clean at home. Available on Amazon.
Fibrous pulpitis
Symptomatology in the fibrotic type is sterile, the pain is weak, more often of a nagging nature. Painful manifestations are mostly noticed after eating, as well as when the affected tooth comes in contact with hot or cold drinks. If fibrous pulpitis is left untreated, the pain may occur regularly and persist for several days. In this case, the pain syndrome increases at night, body temperature may rise, and the discomfort does not disappear even after the elimination of the irritating factor.
Gangrenous
Pain of a predominantly nagging nature, arising from contact with cold or hot food. Over time, an unpleasant putrid odor appears in the mouth, severe pain occurs when pressing on the infected tooth, and a fistula is formed. The gums in the affected area are swollen and red, and the tooth enamel darkens.
Hypertrophic
A rare disease that occurs in an open carious cavity. The pain syndrome is mild, aching in nature, intensifying when chewing food. Many patients have bleeding gums. In the absence of therapeutic measures, hypertrophic pulpitis develops into a chronic form, after which a polyp is formed, fused to the surrounding tissues.
Concurrent
Most often develops due to a large number of pathogenic deposits, which subsequently begin to replace the internal tissues of the infected dental unit. The inflammatory process occurs due to improper treatment of dental pathologies or after mechanical trauma to the pulp. The disease can also develop against a background of diabetes, osteoporosis and poor oral hygiene. Symptoms are a painful reaction to cold and hot or when pressing on the affected tooth.
Traumatic
Occurs less frequently than infectious, mainly diagnosed in children. Causes of traumatic pulpitis are chips, cracks, broken teeth, and burns of the gum tissue. It manifests as painfulness when the tooth unit comes into contact with low or high temperatures.
Warning. Many types of pulpitis are accompanied by identical symptoms, but there are some differences. In the acute course, the tooth usually reacts painfully to low temperatures. If the pathology has acquired a chronic form, the patient feels severe pain on contact with hot food and drinks.
Exacerbation
Chronic pulpitis is often asymptomatic or with minor painful manifestations, but sooner or later the patient expects an exacerbation of the pathology. In addition to the fact that it is unbearably painful, it is also dangerous with various complications (abscess, sepsis).
Two types of chronic pulpitis are prone to exacerbations – gangrenous and fibrous. The symptomatology is manifested in the form of sudden pain, regularly occurring both during the day and at night. Often the pain syndrome radiates to the ears, back of the head, or temporal area.
Causes:
- hypothermia;
- Infectious diseases of the intestines, respiratory tract, and other organs;
- decreased immunity;
- Frequent contact of the affected tooth with cold, hot, or overly hard food.
While the patient is self-treatment and postponement of the visit to the doctor, the destructive process rapidly progresses. After the suppuration of the roots and tissue death begins, we are no longer talking about the removal of pulpitis, but about saving an infected tooth.
Important! Folk remedies for pulpitis are ineffective, so their uncontrolled use will not lead to anything good. Before taking any medication, make sure that you have an appointment with your dentist.
Diagnosis
At the first appointment, the dentist conducts a thorough examination, and during the conversation finds out the nature of the pain syndrome, how long ago it appeared, under what circumstances.
The purpose of instrumental diagnosis is to identify the carious cavity, assess the degree of softening of the pulp, as well as the general condition of the soft tissues.
After that the patient is sent for X-ray examination, which can help to determine the severity of the pathological process, its localization and the size of the lesion. X-ray refers to an informative technique, because after receiving the results, the doctor can determine the condition of not only the external tissues, but also internal structures, including deep root canals.
Sometimes electroodontodiagnostics is performed to confirm the diagnosis. The procedure is based on the analysis of the reaction of the affected tooth to electrical waves. During the study, the doctor determines the integrity and function of the nervous system. In the absence of pathology, the pulp responds to the current passing through it with minor discomfort. If the patient develops caries, the sensitivity of nerve fibers decreases, so there may be no reaction.
Important! Electrodontodiagnostics is not performed if the patient wears a pacemaker, has an intolerance to electric current or is diagnosed with any degree of mental disorders.
Treatment
Modern dentistry uses two types of pulpitis treatment – conservative and surgical. The goal of both techniques is to restore full function to the affected tooth.
Therapy resembles the methods used to eliminate caries, only with pulpitis, more emphasis is placed on the medical treatment of pathological foci. For this purpose, antiseptic drugs, broad-spectrum antibiotics and other medications are used, depending on the symptomatology.
Conservative (biological) treatment
Effective at the initial stages and is carried out in several stages. At the first appointment, the patient is injected with anesthetic, then the cavity is opened. After a thorough treatment with antiseptics, a sterile sponge with antibiotics is applied, and a special fixation dressing is placed on top.
At the second appointment, the doctor treats the tooth cavity thoroughly with medications, and then fills it with a paste, which stimulates the production of hard tissue. A temporary filling is then placed for 5-7 days.
During the third visit to the dental office, the crown portion of the dental unit is filled.
Surgical method
Surgical intervention is performed in stages and is used if conservative therapy is ineffective.
Stages of the surgical method:
- Introduction of anesthesia.
- Removal of the affected tissues from the carious cavity.
- Partial or complete removal of the pulp.
- Thorough treatment of the cavity with antiseptics.
- Injection of medications.
- Filling the root canals and the crown.
If the condition of the infected tooth unit allows, treatment can be performed in one session. We are talking about a pathological process without serious damage and deep tissue damage.
Severe degrees of the disease will require treatment in several stages. At first the cavity is treated and treatment paste is placed under the temporary filling. After 5 days, if there are no complaints there is a repeated antiseptic treatment, and only after that a permanent filling is placed.
During the recovery period, regular oral hygiene, a diet that excludes hard, spicy, fried and salty foods, as well as irrigation of the gums with herbal decoctions or pharmaceuticals is recommended.