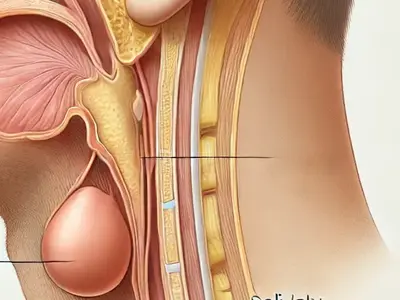
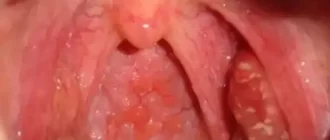
What exactly is parotitis, and why should you care if your parotid gland is swollen? Parotitis is the inflammation of the parotid glands, which are the largest of the salivary glands located just in front of your ears. These glands play a crucial role in saliva production, which helps in digesting food and keeping the mouth hydrated. When these glands swell, it can be painful, visibly noticeable, and potentially serious.
Why Does the Parotid Gland Swell?
There are several reasons why the parotid gland might swell, but one of the most common causes is an infection. A bacterial or viral infection, such as mumps, is often behind parotitis. Mumps, a contagious viral infection, was once a common cause of parotid swelling but has become less frequent thanks to vaccination efforts. However, bacteria such as Staphylococcus aureus can also lead to parotid gland infection, especially in individuals with poor oral hygiene or dehydration.
Pro Tip: This Portable Water Flosser is up to 50% more effective than traditional floss and can save you hundreds on professional dental cleanings. Its 300ml tank and cordless design make it perfect for maintaining healthy gums. Check the current deal on Amazon.
Other causes include obstruction due to salivary stones, autoimmune disorders like Sjögren’s syndrome, or even tumors—both benign and malignant.
Age Groups Affected by Parotitis
| Age Group | Percentage of Cases (%) |
|---|---|
| Children (0-12 years) | 20% |
| Teenagers (13-18 years) | 15% |
| Adults (19-64 years) | 40% |
| Seniors (65+ years) | 25% |
This histogram illustrates the age groups most affected by parotitis, highlighting that adults are most frequently impacted, followed by seniors and children.
Did You Know?
Dental Care: This Rotating Electric Toothbrush removes up to 400% more plaque than a manual brush. With a built-in pressure sensor and 8 replacement heads included (a 2-year supply), it’s a cost-effective way to maintain a professional clean at home. Available on Amazon.
Mumps used to be one of the leading causes of parotid gland swelling until the MMR vaccine became widespread in the 1960s. According to the CDC, mumps cases dropped by over 99% since the introduction of vaccination (source).
How Common Is Parotitis?
The occurrence of parotitis has shifted over the years. Thanks to improved hygiene and vaccination, acute cases due to viral infections have dramatically decreased. However, chronic parotitis, often related to blockages or autoimmune diseases, still affects thousands of people each year.
A study published in the Journal of Oral and Maxillofacial Surgery found that chronic parotitis accounts for about 15-20% of all salivary gland conditions treated surgically. This makes it one of the more prevalent issues when it comes to salivary glands.
Types of Parotitis
| Type | Description |
|---|---|
| Acute Bacterial Parotitis | Typically caused by bacteria; characterized by rapid onset of pain and swelling. |
| Viral Parotitis | Commonly associated with mumps; swelling in both glands is often seen. |
| Chronic Parotitis | Often due to blockage or autoimmune issues; more subtle symptoms. |
Complications of Parotitis
| Complication | Percentage of Cases (%) |
|---|---|
| Abscess Formation | 30% |
| Chronic Inflammation | 40% |
| Dry Mouth (Xerostomia) | 20% |
| Facial Nerve Damage | 10% |
This histogram illustrates the potential complications of parotitis, with chronic inflammation being the most common complication.
What Are the Symptoms?
The symptoms of parotitis can vary depending on the underlying cause, but they often include:
- Swelling: This is usually localized to one or both sides of your face, just below the ears.
- Pain: The swelling can be tender, especially while chewing or opening your mouth.
- Redness and Warmth: The skin over the gland might be red and warm to the touch.
- Dry Mouth: If the gland isn’t producing saliva properly, you might experience a dry mouth, which can lead to further complications.
- Fever: If an infection is present, fever might occur as your body tries to fight off the invader.
How Is Parotitis Treated?
The treatment for parotitis largely depends on what’s causing the swelling. Bacterial infections are usually treated with antibiotics. In some cases, warm compresses and massage may be used to encourage saliva flow and relieve discomfort.
If the cause is a salivary stone blocking the duct, your healthcare provider might recommend measures to dislodge it, such as sucking on sour candies to increase saliva production or even a minor surgical procedure.
For chronic cases, particularly those linked to autoimmune disorders, management is more complex and may include medications to address the underlying autoimmune activity or to alleviate the symptoms.
Success Rate of Parotitis Treatment by Method
| Treatment Method | Success Rate (%) |
|---|---|
| Antibiotics | 85% |
| Surgical Intervention | 70% |
| Warm Compress and Massage | 50% |
| Saliva Stimulation Techniques | 60% |
This histogram shows the success rate of different treatment methods for parotitis, with antibiotics being the most effective.
Did You Know?
Salivary stones, known medically as sialoliths, are the most common cause of blockages in the parotid gland. Up to 80% of all salivary stones form in the submandibular gland, but those that form in the parotid can often lead to significant swelling and discomfort (source).
What Are the Risk Factors?
Certain factors can increase your risk of developing parotitis. These include dehydration, which reduces saliva production and makes it easier for bacteria to infect the gland, and poor oral hygiene. People with chronic conditions like diabetes or those taking medications that reduce saliva flow (such as certain antihistamines or antidepressants) are also at increased risk.
Preventing Parotitis
While not all cases of parotitis are preventable, there are some steps you can take to reduce your risk:
- Stay Hydrated: Drinking plenty of fluids helps keep saliva flowing and reduces the chance of infection.
- Practice Good Oral Hygiene: Regular brushing, flossing, and dental check-ups can reduce the risk of bacterial infection.
- Manage Underlying Health Conditions: Conditions like diabetes can affect your overall oral health. Keeping them well-managed can help prevent complications like parotitis.
When to See a Doctor
If you notice swelling around your jaw or under your ears that doesn’t go away or is accompanied by pain, fever, or difficulty opening your mouth, it’s time to see a healthcare provider. In most cases, parotitis is treatable, but catching it early can prevent complications.
Our Editorial Advice
Parotitis can be uncomfortable and sometimes painful, but understanding the underlying cause is the first step toward finding relief. Keeping yourself hydrated, maintaining good oral hygiene, and being mindful of any unusual symptoms are all ways to stay ahead of potential issues. If you experience persistent swelling or pain, don’t hesitate to seek medical guidance—early intervention can make a world of difference.