Temporomandibular dysfunction consists of a vast array of disorders that often overlap. They include muscle issues that impact jaw movement, pain in the face around the jaw joint, problems within the joint itself.
This variety makes diagnosis and treatment tough. A precise diagnosis is vital for successful treatment. For instance, patients with a muscle problem that is triggering pain will more than likely not take advantage of surgery on the temporomandibular joint (TMJ). Inquire about your doctor’s experience in identifying and dealing with TMJ and facial pain.
A lot of problems, whether muscular or within the joint, get better over time. For this factor, a lot of professionals agree that it’s best to use conservative treatment initially. However in some instances, surgery or other procedures, such as injections, might be recommended as a first treatment.
Pro Tip: This Portable Water Flosser is up to 50% more effective than traditional floss and can save you hundreds on professional dental cleanings. Its 300ml tank and cordless design make it perfect for maintaining healthy gums. Check the current deal on Amazon.
When Does TMJ Require Treatment?
Many people with TMD have temporary symptoms that are not severe and do not become worse. They typically can improve with basic TMJ treatments done at home. In some cases symptoms go away without any treatment at all. They likewise can come back without warning.
If you have TMD, your dental expert might recommend the treatments listed below. Many dentists agree that these treatments work best in mix. You may not get relief using just one.
TMJ Home Treatment Options
Soft foods
If you eat food that does not require a lot of chewing, your jaw gets a possibility to rest and heal. This means you shouldn’t eat food that is:
Dental Care: This Rotating Electric Toothbrush removes up to 400% more plaque than a manual brush. With a built-in pressure sensor and 8 replacement heads included (a 2-year supply), it’s a cost-effective way to maintain a professional clean at home. Available on Amazon.
- Thick or large, requiring you to open your mouth wide
- Chewy, like a caramel apple
- Tough or crispy, like a tough roll, pretzel or raw carrot
When possible, cut food into really small pieces so it’s much easier to chew. The best food to eat, nevertheless, is soft and requires little or no chewing. Examples include:
- Yogurt
- Mashed potatoes
- Home cheese
- Soup
- Rushed eggs
- Fruit smoothies
- Cooked vegetables or fruits
- Fish
- Grains
- Beans
Some people’s symptoms go away after about two or 3 weeks on a soft-food diet. Other individuals need to adhere to this diet for a longer time.
Ice packs, exercise and moist heat
Some individuals discover that a routine of moist heat, exercise and ice helps TMD symptoms. Start by using damp heat to the side of your face and temple. This relaxes tight muscles that might be causing spasms. Try to do this for about 10 minutes. Then do a couple of simple stretching exercises, like this one:
- Put your left thumb under your upper front teeth.
- Put your right index and middle fingers on top of your lower front teeth.
- Carefully pull the jaw apart using your hands, not your jaw muscles.
Your dentist might suggest other exercises, too. End the routine by using ice to the side of your face for about 5 minutes. Try doing this several times a day. Physical therapy often plays an important function in treating patients with TMD. Your doctor might choose to refer you to a physiotherapist.
Medicine
This can consist of:
- Nonsteroidal anti-inflammatory drugs (NSAIDs), such as aspirin or ibuprofen (Advil, Motrin), aid ease muscle pain and swelling. Many can be bought over the counter at pharmacies and supermarket.
- Muscle relaxants help loosen tight jaw muscles. These can be helpful to people who grind or clench their teeth.
- You will need a prescription.
- Antianxiety medicines assist alleviate the stress that is often thought to make TMD even worse. These medications are often used for a short time. They are readily available only with a prescription.
- Antidepressants can be used in low doses to lower or control pain. In these doses, however, the drugs do nothing for depression.
Splints
Splints are designed to fit over the teeth. They prevent the upper and lower teeth from coming together. This makes it hard for you to grind or clench your teeth. These devices take pressure off the jaw joints and muscles so they can unwind and recover. If your dental practitioner believes a splint would assist you, he or she will figure out when you need to use it (during the day or at night) and for how long. A splint must never be worn so long that it alters your bite. If a splint causes or increases your pain, stop utilizing it and contact your doctor.
None of these treatments is a treatment, however they might eliminate the symptoms of TMD. If symptoms continue or return, make sure to see your dental practitioner.
TMJ Pain Treatment
Here are some more suggestions that might help relieve your TMJ pain or discomfort:
- Yawn and chew (particularly gum or ice) as little as possible.
- Prevent extreme jaw movements, such as yelling or singing.
- When you have to yawn, place a fist under your chin and press up. This can keep your mouth from opening too wide.
- Attempt to keep in mind to keep your teeth somewhat apart as typically as you can. Keep in mind that it is natural for your jaw to open a little if your lips are closed.
- Sleep on your back, not on your stomach.
- Don’t rest your chin on your hand or hold the telephone in between your shoulder and ear.
- Attempt to minimize stress.
Other TMJ Treatment Options
There are several types of treatments for TMJ disorders. If your TMD is not better after attempting the basic treatments listed above, your dentist might suggest one or more of the following:
Transcutaneous electrical nerve stimulation (TENS)
This therapy uses low-level electrical currents to unwind the jaw joint and facial muscles. For some individuals, this relieves pain. This treatment can be done at the dentist’s workplace or at home.
Ultrasound
Ultrasound treatment is deep heat that is normally applied to the joint if it aches or does not move. It is typically used in addition to physical therapy.
Trigger-point injections
For this therapy, a dental practitioner injects pain medicine or an anesthetic into tender facial muscles to ease pain. While the pain medicine is working, you should extend your jaw muscles with simple exercises.
Acupuncture
For some people with TMD, acupuncture can be helpful.
Surgery and TMJ Treatment
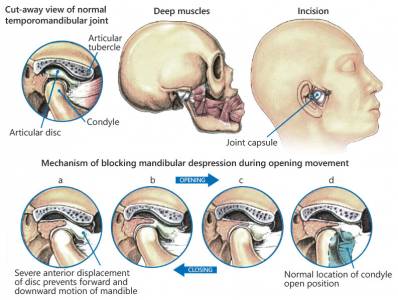
Surgery is generally thought about just if you have attempted all other treatment choices and still have consistent pain and practical problems such as minimal opening of the jaw. Your dental practitioner and oral surgeon also need to have figured out that your TMD is caused by a structural issue within the jaw joint. For instance, you might have limited jaw motion since of displacement of the disk that sits in the jaw joint.
In some instances, surgery is the first option. Patients who have severe degenerative disease might not respond to more conservative procedures.
Prior to having any surgery, be sure to obtain a consultation from another surgeon. Keep in mind, surgery can’t be reversed. It has actually been successful for the most parts, but it sometimes leads to more pain and jaw damage. Be sure your surgeon plainly explains why you need to have surgery, the risks and advantages, and other treatment options. You must have a clear understanding about what you can anticipate from surgery. Likewise, ask about your surgeon’s experience with this type of surgery.
The temporomandibular joint (TMJ) is a small ball-and-socket joint. It consists of the following parts:
- The ball, called the condyle, which is the top part of the jaw bone
- The socket, called the glenoid fossa
- A small, fibrous disk that sits between the condyle and the glenoid fossa
There are two primary types of surgery for TMJ: arthroscopy and open joint surgery.
1) Arthroscopy
Like lots of types of surgery, arthroscopy generally needs general anesthesia. While the patient is unconscious, the surgeon makes an extremely little cut in front of the ear. A little, thin instrument geared up with a lens and light is inserted. The instrument is connected to a video screen and display. This allows the surgeon to analyze the TMJ and surrounding area. Depending on the cause of the TMD, the surgeon may eliminate tissue or change the disk or the condyle. A second incision is then made. The surgeon uses this cut to put little instruments.
3) Open joint surgery
There are lots of types of open joint surgical treatments. In all of them, the surgeon runs on the TMJ without making use of special devices like video displays. Rather, an incision is made simply in front of the ear and the joint is run on under direct vision. Your oral surgeon might recommend this kind of surgery if:
- Your problem can not be remedied with arthroscopy
- Your TMJ is degenerating
- You have tumors in or around your TMJ
It takes longer to heal from this type of surgery than it does from arthroscopy. Although there is a possibility of scarring, the cut normally recovers effectively and is challenging to discover. Your surgeon will discuss other risks of surgery.
A very little part of patients need total joint replacement to remedy the underlying issue.