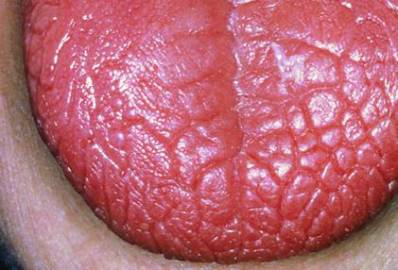
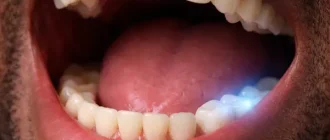
Glossitis (it’s a medical term of beefy red tongue) is typically identified by an inflammation of the tongue. It can also trigger changes in the tongue’s texture and color (usually beefy and red).
As small as it is, the tongue is among the strongest muscles in your body, especially when chewing and swallowing food. And although five-year-olds use it to express their disapproval, it’s vulnerable to certain conditions of its own. For example, if you have anemia, tongue function and look can feel the results nearly as much as your energy level. This condition also known as beefy red tongue.
What Is Beefy Red Tongue?
Likewise referred to as glossitis or anemia tongue, this condition causes beefy red tongue to end up being irritated, and is defined by a number of things when your iron levels are low. The tongue’s look can change into multiple tones of red, and swell slightly in size. The surface of the tongue can ravel and hide its natural texture, as well. These little bumps you feel on your tongue — likewise referred to as papillae — play an important function in the eating process, and countless taste buds are housed inside them. Papillae alteration can affect how you eat and speak.
Pro Tip: This Portable Water Flosser is up to 50% more effective than traditional floss and can save you hundreds on professional dental cleanings. Its 300ml tank and cordless design make it perfect for maintaining healthy gums. Check the current deal on Amazon.
Glossitis can mean soreness of the tongue, or more usually inflammation with depapillation of the dorsal surface of the tongue, leaving a smooth and erythematous (reddened) surface. In a wider sense, glossitis can mean inflammation of the tongue generally.
Wikipedia
Beefy Red Tongue Symptoms and Signs
If you believe you’re experiencing beefy red tongue, schedule a visit with your dental professional so she or he can effectively detect you. Here are some traits to search for before making the call:
- Swollen tongue
- Change of tongue color into beefy-red
- Difficulty or failure to chew, swallow or speak
- Tongue pain and inflammation
- Decrease in or loss of tongue papillae
What Causes Beefy Red Tongue?
A range of conditions can cause beefy red tongue, some more common than others. According to the National Library of Medicine, these consist of:
- Allergies. Medications, hot or hot foods as well as certain types of mouth care items can aggravate the tongue’s papillae. Solutions may for that reason replace a less-sensitive mouth rinse.
- Injuries. Any sort of mouth injury arising from burns or the use of oral appliances like dentures can irritate the tongue.
- Oral herpes. Particular diseases, such as oral herpes simplex, can cause blisters, swelling and tongue pain.
- Dry mouth. Saliva is a need to keep the tongue moist and free of bacteria that can intensify the tongue’s surface area.
Of course, the low iron levels specifying anemia are your first stop. Iron aids the body in making red blood cells. When you’re deficient in them, the tongue’s tissue gets a lack of oxygen, similar to the rest of the body.
Dental Care: This Rotating Electric Toothbrush removes up to 400% more plaque than a manual brush. With a built-in pressure sensor and 8 replacement heads included (a 2-year supply), it’s a cost-effective way to maintain a professional clean at home. Available on Amazon.
Vitamin B12 and Beefy Red Tongue
Vitamin B12 deficiency, which may trigger major neuropsychiatric damage, is typical in the elderly. The non-specific scientific functions of B12 deficiency and unreliable serum parameters make medical diagnosis tough. We aimed to evaluate the worth of oral “beefy red” spots as a scientific marker of B12 deficiency.
How does it checked: A diagnostic research study was performed in patients complaining of oral discomfort, burning sensation, or severe recurrent oral ulcers. Patients underwent clinical assessment and lab examinations, including complete blood count and estimation of serum B12, folate, iron, and ferritin levels. Resolution of medical symptoms and signs after 1 month of B12 supplement was considered the diagnostic gold standard.
Of 136 patients, 70 had B12 deficiency. Among these patients, the oral “beefy red” spot was observed in 61, abnormal mean corpuscular volume (MCV) was kept in mind in 30, and serum cobalamin levels less than 200 and less than 350 pg/mL were seen in 59 and 67 cases, respectively. The “beefy red” patch demonstrated the highest diagnostic validity (Youden index 0.84) and dependability (consistency 91.9% [95% CI: 87.3%-96.5%], followed by the serum cobalamin levels and MCV. The combination of “beefy red” patch with cobalamin less than 50 pg/mL displayed much better diagnostic value than the combination of “beefy red” spot with cobalamin less than 200 pg/mL, with precision of 0.81 vs 0.74 and reliability of 90.4% (95% CI: 85.5%-95.4%) vs 86.8% (95% CI: 81.1%-92.5%).
The combination of oral “beefy red” patch and serum cobalamin level <350 pg/mL seems helpful for medical diagnosis of B12 deficiency.
Smooth Beefy Red Tongue and Gastrointestinal Problems
Roughly 50% of patients have a smooth tongue with loss of papillae. This is generally most marked along the edges of the tongue. The tongue may hurt and beefy red. Occasionally, red spots are observed on the edges of the dorsum of the tongue. Patients may report burning or discomfort, most particularly on the anterior third of the tongue. These symptoms may be connected with changes in taste and anorexia nervosa.
Patients might report either constipation or having numerous semisolid defecation daily. These symptoms have actually been credited to megaloblastic changes of the cells of the intestinal mucosa.
Nonspecific gastrointestinal (GI) symptoms are not uncommon and consist of anorexia, nausea, throwing up, heartburn, pyrosis, flatulence, and a sense of fullness. Rarely, patients present with extreme abdominal pain related to stomach rigidness; this has actually been associated to spine pathology. Venkatesh and coworkers report the case of a patient who provided with epigastric pain, diarrhea, and throwing up and was discovered to have thrombosis of the portal, exceptional mesenteric, and splenic veins due to hyperhomocysteinemia secondary to pernicious anemia.
Types of Glossitis
Tongue inflammation resulting from anemia can take a few different shapes:
- Acute Glossitis. Usually the result of an allergy, this kind of glossitis starts all of a sudden and is accompanied by more noticeable symptoms.
- Chronic Glossitis. This leads to a consistent swelling of the tongue and may arise from another health condition.
- Idiopathic Glossitis. Journal of Medical Reports specifies that this form of glossitis may be linked to celiac disease. Its origin is unidentified, but can cause swelling of the tongue mucous membrane and muscle.
- Atrophic Glossitis. The tongue looses its initial color leading to a dark-red tongue. This form likewise leads to a loss of a great deal of papillae.
Treatment for Beefy Red Tongue
A trip to your dental expert is the best place to begin if you believe you have anemia tongue. During a test, your dental practitioner will search for blisters, an absence of papillae and any signs of swelling on your tongue. Blood and saliva samples might likewise be requested for further testing.
At home, antibiotics, diet changes and correct oral care are all kinds of treatment you can use to combat glossitis. Keep in mind a healthy mouth begins with excellent brushing and flossing. Keep your teeth and gums as healthy as they can be, and being anemic will not imply remaining in oral pain.
Medications
Antibiotics and other medications that eliminate infections might be recommended if bacteria exist in your body. Your medical professional might also prescribe topical corticosteroids to lower the soreness and discomfort.
Home care
Brushing and flossing your teeth several times a day may improve the health of your tongue, gums, and teeth. This can assist alleviate the symptoms connected with glossitis and prevent the condition from happening once again.
Prognosis for Beefy Red Tongue
In many cases, glossitis disappears with time or treatment. Treatment might be more successful if you prevent foods that cause inflammation of the tongue. Practicing appropriate oral hygiene might also help lower or prevent issues. Talk to your doctor if your symptoms do not enhance with treatment or continue to happen.
Call 911 or go to the healthcare facility immediately if your tongue becomes severely swollen and begins to block your airway. This might be an indication of a more serious condition.